VACCINES:
1) “Most people in the poorest countries will need to wait another two years before they are vaccinated against COVID-19,” researchers estimate, according to a story by T. V. Padma for Nature (7/9/21). The story links to this Our World in Data page, which stated on 7/19/21 that 25.9% of the world population has received at least one dose of a COVID-19 vaccine. Only 1% of people in low-income countries have received at least one such dose, the page states: https://www.nature.com/articles/d41586-021-01762-w.
2) In the U.S., UK, and Israel, an increasing proportion of new SARS-CoV-2 infections are occurring among unvaccinated people, most of whom are young, according to sources in Smriti Mallapaty’s 7/8/21 story for Nature. The shift reflects strategies of prioritizing COVID-19 vaccination and other prevention measures in older people, the story states. The "overall risk of severe [COVID-19] in children remains low,” Mallapaty writes. But the trend also means it is now more important to understand SARS-CoV-2 transmission and COVID-19 in children, the story states. The trend also raises questions about how COVID-19 vaccines are distributed worldwide, an Emory University infectious-diseases researcher is quoted as saying: https://www.nature.com/articles/d41586-021-01862-7.
3) A federal advisory panel that advises the U.S. Centers for Disease Control on immunizations is set this week to discuss "whether health care workers should be allowed to give additional coronavirus shots to patients with fragile immune system,” report Lena H. Sun, Yasmeen Abutaleb, and Laurie McGinley at The Washington Post (7/15/21). This extra-shot discussion addresses findings that immunocompromised people who receive the standard dose(s) of COVID-19 vaccines tend to produce fewer antibodies to SARS-CoV-2 than the general population does. The immunocompromised population includes people in treatment for cancer, people who have transplanted organs, and people living with HIV or leukemia. Watch out for how the media and others use the word “booster” — some experts say that once a manufacturer’s vaccine against a disease is tweaked or updated, it’s no longer a booster. It’s a new vaccine. For instance, we don’t usually refer to each year’s updated seasonal flu shot as a booster. Similarly, in the Washington Post story, Dr. Francis Collins, director of the U.S. National institutes of Health, says an additional COVID-19 vaccine dose for people with weaker immune systems isn’t a booster. Instead, “I would call that trying to get the primary immunization into the effective place,” he is quoted as saying: https://www.washingtonpost.com/health/2021/07/15/covid-booster-shots-immunocompromised/.
BREAKTHROUGH INFECTIONS:
4) More than 99 percent of COVID-19 hospitalizations in the U.S. are now among people who are unvaccinated against the disease, Dr. Daniel Green said on the 7/17/21 episode of This Week in Virology. Still, a small percentage of vaccinated people in the U.S. can get infected with SARS-CoV-2 (“breakthrough infections”) and a small percentage of that group dies. Per this 5/28/21 report by the U.S. Centers for Disease Control (CDC): "Even though [U.S. Food and Drug Administration]-authorized vaccines are highly effective, breakthrough cases are expected, especially before population immunity reaches sufficient levels to further decrease transmission. However, vaccine breakthrough infections occur in only a small fraction of all vaccinated persons and account for a small percentage of all COVID-19 cases”. More data on breakthroughs as of April 30, can be found in the CDC post: https://www.cdc.gov/mmwr/volumes/70/wr/mm7021e3.htm.
5) Katelyn Jetelina at Your Local Epidemiologist suggests in a 7/16/21 post that the following factors may increase your chances of a “breakthrough infection”: a) age — older adults are less protected by the vaccines; b) a weaker immune system, due to immune-suppressing drugs etc., c) exposure to a larger dose of the virus — e.g. spending extended time with an infected person in an unventilated area, likely indoors, d) spending extended time in communities with low vaccination rates, and e) exposure to the delta variant that’s now widespread in the U.S., UK, and India. The Pfizer, Moderna, and Johnson & Johnson vaccines seem to be a little less effective against delta than they are against the original strain of the virus: https://yourlocalepidemiologist.substack.com/p/how-many-breakthrough-cases-are-there.
6) A 6/23/21 story by Johnny Diaz at The New York Times offers some tips for vaccinated people who test positive for SARS-CoV-2. The tips are fairly similar to the guidance for people who got infected before vaccines were available: 1) isolate from others to prevent spreading the virus, 2) inform your doctor as well as anyone you were in recent, close contact with so they can get tested and take precautionary measures (the details here are vague), 3) at home, stay in a separate room from any house-mates, don’t share dishes and towels, and use a separate bathroom, if possible, and 4) open windows and use fans to ventilate the home. You probably won’t infect others, says a physician at Northwell Health. “The level of virus in the nose and droplets are not as contagious in a vaccinated person,” he is quoted as saying: https://www.nytimes.com/2021/06/23/us/can-i-get-covid-after-the-vaccine.html.
7) I’ve been involved in some conversations about the media coverage of SARS-CoV-2 breakthrough infection reports. Questions include whether the media is over- or under-covering breakthroughs and whether these stories significantly contribute to vaccine hesitancy. For example, here’s a 7/19/21 story by Amanda Kaufman at the Boston Globe about a cluster of breakthrough cases in Provincetown, Massachusetts, a beautiful beach town that is well-known for large social gatherings at bar and parties and in restaurants. A significant portion of these gatherings will be indoors, in under-ventilated areas, and/or among unmasked people. I always look for information in these stories about the numbers of symptomatic cases, severe cases, hospitalizations, and deaths in these outbreaks. This Boston Globe story attributes to a county human services staffer that 73% of the 132 reported cases are symptomatic but the majority of symptoms are mild: https://www.bostonglobe.com/2021/07/19/nation/provincetown-issues-new-covid-19-advisory-response-uptick-cases/.
DELTA VARIANT OF SARS-CoV-2:
8) Here is Katelyn Jetelina’s latest chart at her site Your Local Epidemiologist comparing the effectiveness of the various available COVID-19 vaccines against SARS-CoV-2 classic and some of the variants, including the delta variant (7/2/21). The chart is lower down in this post about the antibody response to the Johnson & Johnson vaccine against the delta variant. (Antibody response is important but immune cells called B cells and T cells also contribute our immune system responses to illness-causing bacteria and viruses. They are often left out of the conversation, in part because they are harder to measure. See Katherine J. Wu’s explainer in the 2nd to last section of the newsletter, below). Jetelina’s conclusion: “yes, the J&J vaccine still works, to some degree, against delta. You are protected”: https://yourlocalepidemiologist.substack.com/p/j-and-j-and-delta-update.
9) The delta variant is more likely to cause regional outbreaks in areas with low COVID-19 vaccination rates than it is to cause a nationwide surge in infections, according to experts interviewed by Tanya Lewis at Scientific American (6/29/21). “Vaccination remains the best tool for combatting a delta surge,” the story describes experts as saying: https://www.scientificamerican.com/article/how-dangerous-is-the-delta-variant-and-will-it-cause-a-covid-surge-in-the-u-s/.
10) Not all experts agree about how to think about the spread of the delta variant of SARS-CoV-2 in the U.S., UK, India and beyond. Behaviors such as getting vaccinated against COVID-19, mask-wearing indoors, travel, and adherence to social-distance policies are more important drivers of current increases in coronavirus infections than variants are, write Amy B. Rosenfeld and Vincent Racaniello, both virologists at Columbia University (Racaniello hosts the This Week in Virology podcast). In a 6/29/21 essay in The New York Times, Rosenfeld and Racaniello also explain that mutations in a virus affect its fitness (its “ability to reproduce and spread”) and use that to dispute the idea that some of the new variants are more infectious, more contagious, or more deadly. “Just because a variant displaces another does not necessarily mean it is more infectious or more deadly to the people who become infected with it,” the authors write: https://www.nytimes.com/2021/06/27/opinion/covid-vaccine-variants.html.
11) This 7/20/21 story by Brenda Goodman for Medscape rounds up some of the early evidence suggesting that the delta variant of SARS-CoV-2 is more contagious and possibly causes more severe COVID-19 in people who are unvaccinated than the original strain of the virus does. The story’s 2nd page cites a few new interesting studies that shed light on why delta might be more contagious — it might be less vulnerable to antibodies to the virus and more likely to form large clusters of [infected] cells that help the virus make copies of itself, Goodman reports. In reading these stories, I look for information about the fully vaccinated rate in regions where the delta variant has caused a great deal of sickness and death. It seems to often be low or fairly low, if that information is provided: https://www.medscape.com/viewarticle/955116.
MORE PUBLIC HEALTH:
12) It’s legal for employers in all but 6 U.S. states to require vaccinations, and it is not a HIPAA (Health Insurance Portability and Accountability Act) violation if employers ask for your COVID-19 vaccination status, per sources in this helpful 7/14/21 Scientific American story by freelance journalist Christie Aschwanden. The best measure you can take to reduce your risk of infection back at the office: get vaccinated. The COVID-19 vaccines are so effective at preventing severe illness and death that, for people who are fully vaccinated, “it really doesn’t matter what the vaccine status is of those around you,” a Wayne State University infectious disease physician is quoted as saying. Unvaccinated people and those with weakened immune systems “should wear a mask around others who are not in their immediate household (which is usually the case for those in an office), stay six feet apart in public spaces, and avoid crowds and poorly ventilated areas, according to the [U.S. Centers for Disease Control]," the story states. Don’t trust those plexiglas barriers for protection over several hours, the story suggests. They are only useful for short face-to-face interactions like those with bank tellers, Virginia Tech environmental engineer Linsey Marr is described as saying. The story includes details to ask about the rate of air exchange in an office and the minimum efficiency reporting value (MERV) of the heating, ventilation and air conditioning system’s filtration. It should have a MERV rating of at least 11, Marr is described as saying. It sounds like using a portable air filter (with a HEPA filter) isn’t a bad idea either: https://www.scientificamerican.com/article/is-your-office-safe-from-covid-what-to-know-now-that-your-boss-wants-you-back1/.
13) The U.S. Centers for Disease Control’s 7/9/21 updated recommendations for COVID-19 safety in K-12 schools this fall places a lot of responsibility on schools, writes Katelyn Jetelina at Your Local Epidemiologist on the same day. She particularly notes a passage stating that “localities should monitor community transmission, vaccination coverage, screening testing, and occurrence of outbreaks to guide decisions on the level of layered prevention strategies.” But she praises the guidance for including recommendations for testing strategies for students, teachers, staffers, and sports activities, depending on the extent of community transmission. Overall, the plan puts primacy on a return to in-person learning and vaccination for eligible students (currently that means students 12 years and up in the U.S.). Unvaccinated children should wear masks indoors, the guidance states. Schools are expected to maintain 3-feet of distance between students in classrooms: https://yourlocalepidemiologist.substack.com/p/cdc-says-schools-in-session.
14) Subsequently, the American Academy of Pediatrics (AAP), the leading association of pediatricians in the U.S., has recommended mask-wearing among all students over age 2, vaccinated or not, and a full return to in-person classrooms this fall (7/19/21), according to various reports. Francis Collins, director of the U.S. National Institutes of Health, calls the AAP recommendations reasonable, reports Reis Thebault at The Washington Post (7/20/21). “They will not be popular amongst parents and kids who are sick of masks, but you know what? The virus doesn’t care that you’re sick of masks,” Collins told MSNBC, the story states: https://www.washingtonpost.com/health/2021/07/19/aap-mask-schools-vaccination/.
15) Looks like Belgium is leading the way with indoor ventilation requirements related to COVID-19 safety, per these 7/6/21 tweets by Virginia Tech aerosols expert Linsey Marr and atmospheric chemist Jose-Luis Jimenez, of the University of Colorado Boulder:


MORE SCIENCE THOUGHTS AND FINDINGS:
16) This 7/12/21 essay by Robert M. Kaplan at Stanford Medicine’s Clinical Excellence Research Center states that the rapid decline in SARS-CoV-2 infections in the U.S. started before the widespread availability of COVID-19 vaccines. This pattern matches similar outcomes found in past pandemics and disease outbreaks, including for tuberculosis, polio, smallpox, pneumonia, and influenza, Kaplan writes. He credits vaccines with “much credit for declining rates of COVID-19.” But he also thinks that “the protection provided by natural infection has been under appreciated” — that is, immunity acquired by surviving a SARS-CoV-2 infection. A combination of factors led to the case decline this spring in the U.S., the essay states. Kaplan concludes: “Even though vaccines did not initiate the decline in COVID-19 cases, they are the best tool available for assuring that the smoldering fire of it is extinguished”: https://www.statnews.com/2021/07/12/covid-19-decline-preceded-vaccines-still-need-jabs-finish-the-job/.
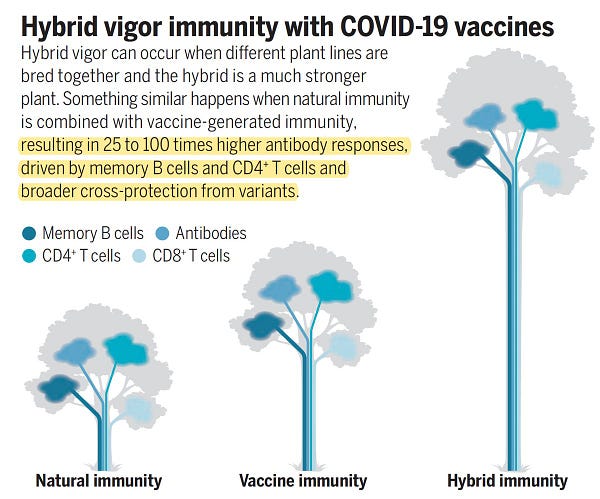
17) This 6/24/21 Twitter thread initiated by Dr. Eric Topol at the Scripps Research Translational Institute alerted me to a 6/25/21 paper in Science by virologist and vaccine researcher Shane Crotty at the La Jolla Institute for Immunology that explores "hybrid immunity” to SARS-CoV-2. The question of hybrid immunity to the novel coronavirus is why people who have had COVID-19 and one dose of an mRNA COVID-19 vaccine (a combination of natural immunity and vaccine-generated immunity) have stronger immunity to SARS-CoV-2 than do people who are fully vaccinated and have not had COVID-19 (that is, just vaccine-generated immunity). I can’t pretend to have understood this entire, short essay, but it’s a fun read if you enjoy learning immunology. And the answer seems to lie primarily in the memory B cells created in response to a SARS-CoV-2 infection. Memory B cells create antibodies that can fight any re-infection with a microbe. But they also “encode a library of antibody mutations” to address variants of that microbe. Wow. Regarding SARS-CoV-2 infections, Crotty writes: “Memory B cells are increased 5- to 10-fold in hybrid immunity compared with natural infection or vaccination alone”:



18) “COVID is low risk for children, but not no risk” — this is a paraphrase of statements Dr. Daniel Griffin often repeats on the podcast “This Week in Virology." Related: A small study published in April study found that more than a third of children diagnosed with COVID-19 have symptoms that linger for four months or more, reports Dyani Lewis for Nature (7/14/21). This finding and others reveal that children, both those who had symptomatic COVID-19 and those who had symptom-free COVID-19, can end up having so-called “long COVID.” Some other estimates for the prevalence of long COVID in children are lower, Lewis reports: https://www.nature.com/articles/d41586-021-01935-7.
19) The biotechnology behind two of the COVID-19 vaccines authorized for use in the U.S.— mRNA that provokes our cells to make “part or all of a protein that causes an immune response” — could soon be used to develop vaccines against other diseases, including the flu, reports Mike May for Nature Medicine (5/31/21). This story came out a couple months ago, but I’m sharing it now because I recently have heard people wonder about the future of mRNA vaccines. Other diseases for which mRNA vaccines are in development include HIV, hepatitis C, malaria, tuberculosis, dengue, rabies, cancer, and the virus that causes genital herpes, ,sources are quoted as saying. “We do not have a platform for every disease, but the great advantage of mRNA vaccines is that we can test novel hypotheses in rapid succession,” a microbiologist at the University of Illinois College of Medicine is quoted as saying: https://www.nature.com/articles/s41591-021-01393-8.
IMMUNE SYSTEM EXPLAINERS:
20) This cute, PG-13 word-less animated video, written by Maya Adam MD, faculty lead for the Global Child Health Media Initiative, illustrates how COVID-19 vaccines work (sound on, ideally):
21) This two-minute video explains how the immune system works to defend against microbes and parasites (sound on): https://www.scientificamerican.com/video/what-is-the-immune-system-and-how-does-it-work/
22) This beautifully written 4/22/21 immune-system explainer by Katherine J. Wu at The Atlantic is one of my favorite COVID-19 science stories: https://www.theatlantic.com/science/archive/2021/04/antibody-breakup/618668/.
ENTERTAINMENT:
23) SOUND ON: https://www.instagram.com/reel/CRJs7ZHHFcO/
24)


25) SOUND ON:
26)


27) SOUND ON:
————
PLEASE CANCEL PATREON DONATIONS TO THIS NEWSLETTER: I no longer wish to receive donations for this newsletter. Please cancel Patreon commitments. Thanks for all the support in the past year, financial and otherwise! I’m still writing this newsletter though. Just with less frequency.
TAG ME: Please reply to this email to send feedback and/or good SARS-CoV-2 or COVID-19 science coverage that you’ve read, written, or produced in English, Spanish, French, etc.
Love/In friendship, Robin



